Dr. Mariette Chartier presents Manitoba Centre for Health Policy study on the rise of chronic kidney disease in Manitoba.
Chronic kidney disease rising in Manitoba: Can we change the future?
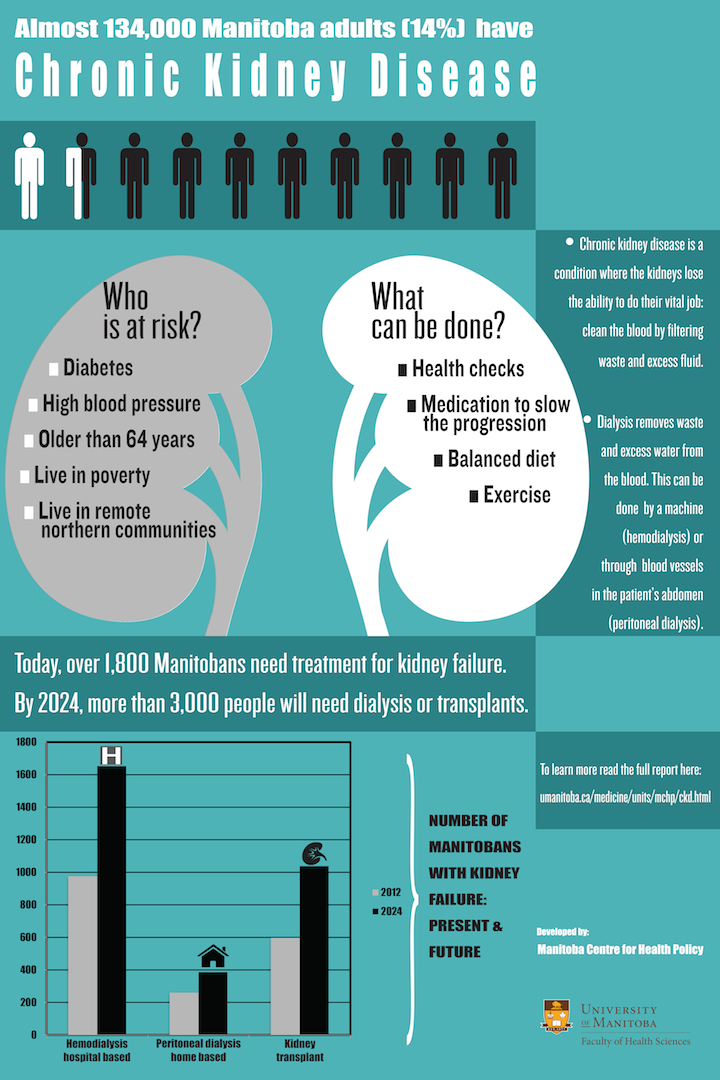
More than 1,800 Manitobans are currently living with kidney failure (the most advanced stage of chronic kidney disease) and according to a new study, this number is on the rise.
Researchers at the Manitoba Centre for Health Policy at the University of Manitoba examined patterns of chronic kidney disease, the need for transplants and dialysis, and how those treatment types differ across the province. They report their findings in Care of Manitobans Living with Chronic Kidney Disease.
The researchers predict a huge increase in cases, estimating that by 2024, more than 3,000 Manitobans will be receiving treatment for kidney failure, either by dialysis or kidney transplant. Most will be using centre-based hemodialysis, which is the most common form of treatment and the most expensive – the cost per person is about $107,000 annually. Fewer people are offered peritoneal and home-based dialysis due to the intensive training that is required.
“Ideally, we would like to see changes in these trends – less centre-based hemodialysis and more peritoneal and home hemodialysis since the home-based options offer patients a better quality of life and result in lower healthcare costs,” says Mariette Chartier, research associate in the U of M’s department of community health sciences and the study’s principal investigator.
Kidney disease is usually caused by other chronic conditions such as diabetes and high blood pressure. Older adults and people living in poverty with poor access to health care and healthy food are more likely to develop kidney disease. In the early stages of the disease, most people do not exhibit symptoms, so an early diagnosis is key to ensure the right care and regular monitoring. Receiving the appropriate care can slow down the disease and help people live longer.
Right now up to 14 per cent of adults in Manitoba have chronic kidney disease, with the highest estimate being 134,000 people. At least one-third of those are at high risk of progressing to kidney failure. These individuals also suffer from many other illnesses: they are five times more likely to have heart disease than adults without chronic kidney disease and nearly 14 times more likely to have a stroke.
Three per cent of children in Manitoba also have chronic kidney disease, which came as a surprise to researchers.
“The real concern is that because chronic kidney disease is progressive, [children] have a longer lifetime risk of kidney failure,” says Chartier. “Unless current patterns change, the increasing number of people with kidney failure will hit Manitoba’s northern and rural communities especially hard.”
While the study did not examine the reasons behind the escalating rates of chronic kidney disease, Chartier said, they are likely attributed to the higher incidence of Type 2 diabetes and poverty, and limited access to health and social services in these communities.
This report recommends a comprehensive public health strategy be put in place to tackle the interrelated health issues, and to address social factors such as poverty and lack of access to healthy food that contribute to these problems.
Research at the University of Manitoba is partially supported by funding from the Government of Canada Research Support Fund.