Rosemary is apologizing for the gruffness of her voice. It’s lower than usual because she’s fighting a cold. The doctor gave her some cough syrup and antibiotics and she’s resting at home.
“I’m hoping,” she says, “that tomorrow morning I can go back and continue to do my work.”
For 17 years, Rosemary has worked in Nairobi’s sex trade, having intercourse with up to 10 men a day, some of them HIV positive. She says she has no idea how many men she’s had sex with, or how many times she’s been exposed to the virus, and yet she remains uninfected.

Photo by Will Swanson
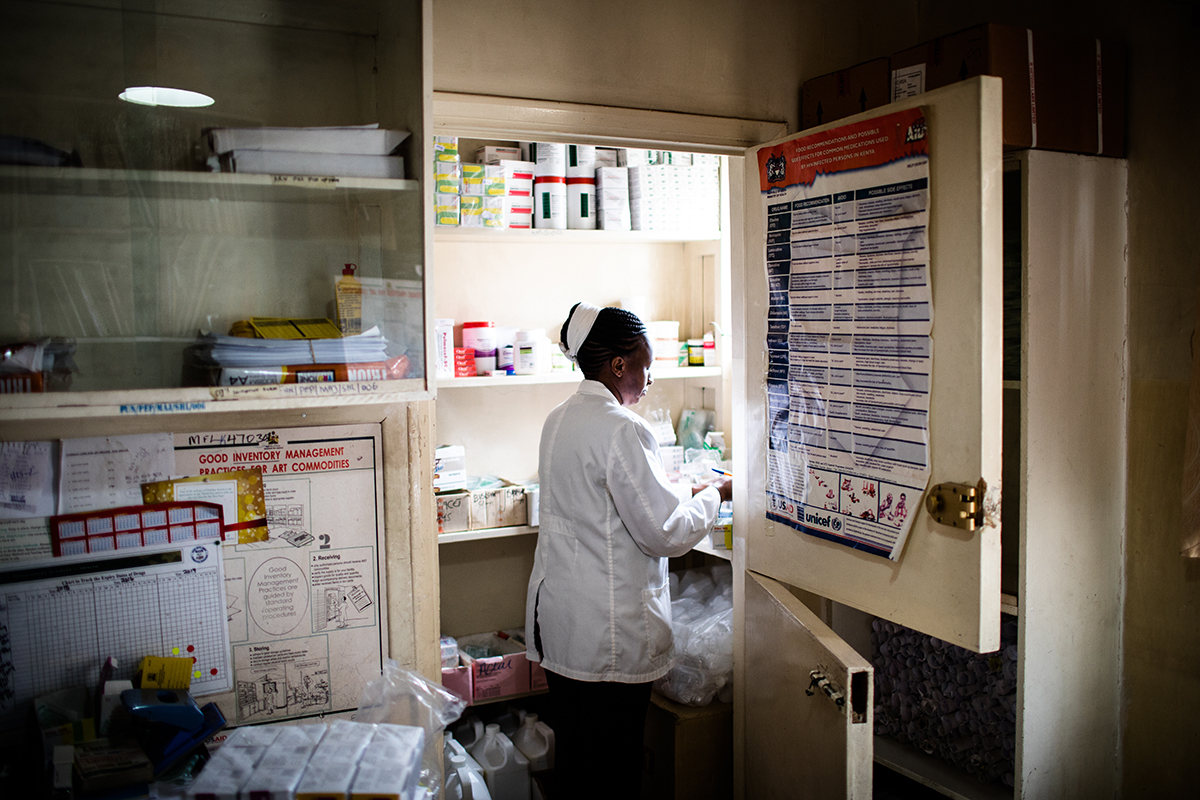
Now she uses condoms and takes a pre-exposure prophylaxis (PrEp) for protection—an intervention introduced in Kenya this year, and one step closer in the lengthy pursuit for a vaccine (it took 47 years to develop one for polio). Rosemary heard about PrEp through the Sex Workers Outreach Program, or SWOP, a University of Manitoba-driven initiative offering testing, treatment and counselling at dedicated clinics in Nairobi County, including Majengo, one of Kenya’s oldest slums.
Rosemary says, flat-out: “If the clinic was not there, half of us would be dead right now.”
The Kenya AIDS Control Project was borne of a decades-long partnership between the University of Manitoba and the University of Nairobi. With millions in funding from the Bill and Melinda Gates Foundation, a team of students and seasoned researchers collect evidence and put lab findings into practice through seven clinics and community sites that reach this key population contributing to Africa’s prevention gap: sex workers.
Rosemary tells me the only reason she agreed to share her story is because her faith in the U of M runs deep. Trust is rare among her clients, among the police.
She is a peer leader with SWOP who advises her circle— especially the youngest and most timid—to insist their clients use condoms and lubricants. She has even travelled with the university to South Africa and India to learn from other women involved in similar HIV-prevention projects.
One of Rosemary’s friends describes her as Powerful. This 45-year-old mother of two who once dreamt of becoming a journalist also advocates against gender-based violence. She likes being the first to know and is a valuable information source for women who want to stay alive in an industry where violence and rape are routine and often by the hand of authority.
Rosemary shares how police officers dropped her three hours away in the middle of nowhere and another time refused to let her out of jail unless she had unprotected sex with them. She has formed an advocacy group to fight back and report violations, and SWOP now does anti-harassment training with police officers.
She sees U of M scientists at the clinic and forums, called “barazas,” that gather hundreds of sex workers to safely share their stories of triumphs and trauma.
A peek into Rosemary’s world: Her sex work shifts go from 7 a.m. to 11 a.m., and again from 11 p.m. to 5 a.m; her office or “hot spot” is a room she rents with no toilet, just a bed, a basin with warm water, a towel and a stool outside where she sits until the next client arrives. She earns $2 CAD per client and as much as $24 from someone who wants her to stay the night, and there’s always a risk they won’t let her go. She says she was once forced to stay for four days. “It’s hard to sleep next to a stranger. Your heart is pumping until morning,” she says.
The first time Rosemary had sex for money she was 23. She remembers the skimpy black mini dress she put on that night. He was a white man, sweaty from the nightclub, and she awkwardly massaged his sticky back. She’s still mad at herself for not having had the courage to insist on collecting more money when he demanded she do more than what they agreed. “I cried,” she says.
To Rosemary, sex work is the only way to support life as a single mom in poverty with no education. Her sons don’t like what she does. It shows when they get moody, she says quietly. Her parents also don’t want to talk about her job when they send for money to buy another sheep for their farm.
But there’s no doubt she’s proud to declare sex work alone is how she made enough money to send both of her sons to college, where one studies agriculture, the other conflict resolution. “I derive a lot of joy and happiness from being with my children,” Rosemary says.
She believes her supporting role with SWOP—which serves more than 30,000 sex workers—is giving her a chance to make her mark, to leave the world “better than she found it.”

Photo by Thomas Fricke
Just like that, he was gone.
When a colleague didn’t show up for work one day, the U of M’s head of medical microbiology and infectious diseases Keith Fowke [BSc(Hons)/88, PhD/95] didn’t think too much of it until he got the phone call.
The Kenyan-born research associate he worked alongside, who trained for some time in Canada, who won awards for his keen intellect, who for years toiled away in the Nairobi lab to move forward the science to stop HIV, had fallen victim to complications from that same virus.
“I didn’t know all the time I worked with him that he was HIV-infected. He was so enthusiastic about research and its potential,” Fowke recalls. “That was quite devastating. It really brought it home: This isn’t a theoretical exercise. And even today there is still rampant stigma and discrimination and many prefer not to disclose their status.”
“I remember grabbing the phone and calling Frank and saying, ‘Our theory was actually right.’”
His colleague succumbed to a secondary infection. HIV can go for the lungs and, despite the advances in medication, a common cure remains elusive.
In the late ’80s, Fowke was a graduate student under medical microbiologist Dr. Frank Plummer [MD/76] when they made a major discovery that significantly advanced the international pursuit of a vaccine. They uncovered that some Kenyan women, all of them sex workers, were somehow immune to HIV despite having been exposed to the virus up to 2,000 times.
Fowke was on the balcony of his Nairobi apartment crunching reams of data he brought home from the lab and couldn’t believe it. “I remember grabbing the phone and calling Frank and saying, ‘Our theory was actually right.’”
The women had natural immunity; their healthy cells were killing the HIV, prompting scientists worldwide—from Sweden to Israel—to explore the phenomenon in others, including heterosexual partners of those infected, gay men and haemophiliacs.
Fowke now knows that the immune cells of the women in the study with this natural resistance are calm or less active and overexpress a protective protein. They know resistance can drop when sex workers take a break, and can run in families.
He is cautiously optimistic the latest breakthrough might come in the form of a simple pain pill. While substantiating the findings is ongoing, he and his team so far have learned that by reducing the presence of the type of cell that HIV targets in the genital tract, they can reduce the chance of infection. Acetylsalicylic acid (better known as Aspirin), his latest research shows, is a way to keep these cells to a minimum. The team’s initial findings show the pill can shrink the number of these cells by 35 per cent. “Then, when HIV does show up, there’s no way for it to get a foothold and initiate an infection,” Fowke says.
They looked at Aspirin since it’s cheap, readily available in developing countries, FDA-approved, already taken daily by cardiovascular and dementia patients and doesn’t require the red tape of a patent. “We just have to provide the solid, scientific evidence that it does prevent HIV infections, and then I think that’ll add to the toolbox we already have in terms of prevention approaches—and hopefully make a difference.”
A decade ago, all eyes were on Germany’s Timothy Brown, the first person cured from HIV. When Brown developed leukemia, doctors essentially killed his immune system with radiation and then put back healthy cells from a donor who happened to have a natural mutation that didn’t allow for HIV infection. Brown has been HIV-negative ever since.
“So that’s been a really important story, that HIV can be eliminated from a single individual,” says Fowke, who belongs to the research consortium CanCURE, a national group formed post-Brown, dedicated to finding a cure. “The problem is, they’ve tried it a number of times [on other patients] and it hasn’t worked. The radiation has been very hard on the patients and some of them have died because of the treatment. For some of them, the HIV has come back. So we now know it’s theoretically possible, but we also know it’s so difficult that it’s not going to be a routine measure that could be used to treat people.”
The other angle to the battle is prevention, a complex task in poverty-stricken parts of Kenya, which Fowke warmly considers his second home. He regularly shares his findings with sex workers there through Swahili translators. He knows their stories well, including that of an HIV-positive woman narrowly saved by the heroic efforts of Winnipeg-based researchers who—in the early days, when funding was for research studies, and not yet treatment— shipped whatever anti-HIV medications they could gather, even meds almost-expired from pharmacies or left in cabinets of people who died.
These women are survivors, Fowke says.
“To see such strength from women living a very poor situation… They’re not poor of spirit that’s for sure.”

photo by Adriane Ohanesian
Dr. Joshua Kimani drops a lot of numbers in casual conversation and they bear a heavy load. 3,000 (his estimate of how many female sex workers he’s known who have died from HIV complications). 90 (the percentage of them who are moms). 100-plus (how many friends, colleagues and family members he’s lost to HIV). 3 (the number of his cousins currently fighting it and doing well).
“They made me who I am. I am able to take care of my community.”
And the most promising: 1. There’s been only one sex worker from the Majengo clinic lost in the last three months—and she died of cancer.
“We used to lose maybe six in a month from HIV. It was horrible. I was the messenger of death and doom,” says the Kenyan-born doctor, a U of M cross-appointed associate professor in medical microbiology and infectious diseases who for two decades has been at the heart of the university’s collaboration with the University of Nairobi, his alma mater.
HIV was at its most hellish pre-2005 when there was no treatment to suppress symptoms. Kimani would give dying patients the cash they needed to go home and be with family in their final days—a heartfelt but also economical gesture since it was less expensive than transporting a coffin.
Today, as clinical director of the U of M/U of N Collaborative Research Group, it’s his job “to make sure the negative remain negative and the positive remain healthy and don’t spread the infection.”
The sex workers are so comfortable with Kimani, they greet him with hugs. He says he’s modelled his in-the-trenches approach to care by watching researchers like Plummer and Distinguished Professor Emeritus Dr. Allan Ronald [MD/61, BSc(Med)/61, DSc/11], who launched the ground-breaking partnership in 1980 and was among the first to study what was then a cryptic new disease. Ronald and the team led landmark studies in the global epidemic of HIV/AIDS and they’ve since trained and mentored more than 500 professionals, including doctors, scientists, peer educators, and PhD students from around the world.
“They made me who I am,” says Kimani, 52. “I am able to take care of my community.”
He grew up in a village 100 kilometres outside Nairobi, home to such extremes in wealth and poverty. He and his brother—sons of a peasant farmer and a nurse—listened to their uncle, a teacher, when he said education was the only way up. Kimani was four when his mom died from a thyroid growth, a mystery he and his brother were able to figure out only once they were in medical school.
As a U of N student, Kimani got an invite to visit Manitoba and it was then he became fascinated by infectious disease and promptly switched his focus from cardiology.
He has helped to bring about a big win: Condom use among female sex workers has gone from virtually nil to 100 per cent with casual clients and 80 per cent with regulars. The team pioneered a sexually transmitted infection management approach that has led to a 65 to 80 per cent drop in classic STIs—and it’s since been disseminated elsewhere, including India.
The program also makes it possible to distribute antiretroviral therapy (or ART), what Kimani calls the “biggest gamechanger of the 20th century.” The medications suppress viral load in those who are HIV positive, reducing the risk of spreading the virus. But getting people to take the drugs is an ongoing challenge.
Female sex workers feel the sting of stigma but their male counterparts perhaps feel it most given same-sex intercourse is criminal in Kenya and punishable by up to 14 years in prison. There are 2,000 male sex workers now involved in SWOP; their incident rate of HIV (at 11 per cent) is five times higher than in the women.
“Gay men have been hiding in the woodwork. They get infected, they hide. By the time they come out, it is too far gone. Those are real issues,” says Kimani.
He shares a poster they use to convince people to come forward and get on ART. It shows a before and after of a young man so emaciated you can count every rib and then with meat on his bones and sparkle in his eyes. One of Kimani’s current studies looks at social media, including Facebook and Grindr, as a way to spread safe-sex messages. “They shut you out but at least they know something,” he says.
There are a dozen HIV-prevention tools informed by decades of research, including the prompt treatment of other sexually transmitted diseases (which Plummer showed increases viral load and transmission risk).
Kimani feels frustrated that, despite the advancements, the greatest challenge remains regressive thinking: It won’t happen to me.

photo by Thomas Fricke
Winnie Apidi treasures her Kenyan tea. As well as her cooking stick she uses to make the cornmeal staple ugali. And the Maasai-inspired red bedspread she’s had since boarding school.
From her Winnipeg apartment, these everyday items connect her to home. The 34-year-old came to the University of Manitoba to do her PhD in medical microbiology and infectious diseases and now splits her time between the Canadian Prairies and the lab in Nairobi while researching the metabolism response within the immune system cells of HIV-resistant sex workers.
She’s deeply intrigued by the phenomenon and is one of dozens to probe the blood sample database of more than 6,000 study participants grown over decades through the U of M/U of N partnership. Roughly five per cent of the cohort is immune.
“It is the largest HIV-resistant cohort in the world. Before, it was this big pool where you would go at it in various directions but the results that have been coming up over the years, people have really narrowed it down,” Apidi says.
The research has become highly specific. Scientists might study a particular gene, protein or sugar in the blood. Apidi’s efforts build on earlier U of M work that mapped genes in the blood of the HIV-resistant women. She discovered they break down sugars normally but these particular genes are under-expressed. “This may be one of the factors that leads them to being resistant—because it’s a combination of factors,” she explains.
Like so many Kenyans, Apidi has lost loved ones to complications from HIV: three aunts and three uncles. Her voice softens, “lots of cousins.”
She was raised in Nairobi but her ancestral home is Kisumu County, where the prevalence of the virus is three times greater than in Kenya as a whole: nearly 20 per cent of the population is HIV-infected. “Previously, if you go there you would find entire families wiped out in some homesteads but due to mass education and prevention measures a lot of progress has been made,” she says.
The average Canadian likely doesn’t grasp the magnitude of HIV/AIDS in Sub-Saharan Africa, Apidi insists. And yet rates are climbing closer to home. (In Saskatchewan, a recent doubling of the national infection rate—mostly through injection drug use—prompted one doctor to call it a state of emergency, and launched a provincial prevention strategy.)
UNAIDS set a goal they’re calling 90-90-90 to help end the AIDS epidemic. By 2020 the aim is that 90 per cent: of all people with HIV will have been diagnosed, of all those diagnosed will be on medication, of all those on medication will have a supressed viral load to reduce the spread.
“This target may look ambitious, but it is achievable with national plans being implemented,” Apidi says. “Kenya is approaching the first target with testing reaching 86 per cent in some populations.”
Right now, 36.7 million people have HIV worldwide.
Will there be a day when there’s no longer a need to talk about it?
“Yes, I believe so. I’m optimistic,” she says. “However, it needs everyone’s hands on deck: the government, the funders, the NGOs, the scientists, the health workers, the people themselves.”

photo by Will Swanson
Joyce Adhiambo makes it clear she will not hide. The HIV-positive sex worker is adamant: “Write my real and actual name.”
“I want the world to hear my story,” she says from her home in the Dandora slums in Nairobi. “I’m very comfortable.”
At 44, she is quick to laugh or break into song as her grandchildren can be heard playing in the background.
Adhiambo is a community advocate within SWOP and one of the first sex workers to share her HIV-positive status at public meetings. It’s a big deal in a community where cultural beliefs and stigma can keep the sick from seeking the medical means to prevent, diagnose or treat a virus that 25 million people in Africa are living with.
Still today some people in her home community believe when they fall ill they are cursed and, instead of seeking help from conventional medical doctors, they go to a witch doctor—a type of traditional healer.
Adhiambo says her father was a polygamist with two wives and believed when he developed a rash and a chronic cough, it was because someone was jealous of his large house and had put a curse on him. He never went to the doctor and died of AIDS.
“He thought he was bewitched,” says Adhiambo.
“I want the world to hear my story.”
Both of her mothers, skinny and sick, eventually died from HIV complications, too. Scientifically sound prevention tools can face scepticism in communities grounded in these deep cultural beliefs. For example, Adhiambo says some people avoid circumcision because they believe the removed foreskin could be used for witchcraft. This despite U of M researcher Dr. Stephen Moses showing that circumcision reduces a man’s HIV risk by 60 per cent. The dramatic finding ultimately earned endorsement from the World Health Organization.
Adhiambo herself followed the doctrine of her community’s beliefs that dictated she leave her husband when he didn’t attend her father’s funeral, and then have unprotected sex with a stranger to “cleanse the family” and ensure her kids would live long lives. She doesn’t know if that was the time she contracted HIV. She got into sex work shortly after to support her three kids and when diagnosed in 2002 still didn’t know how to use a condom.
Adhiambo turned to alcohol to cope and it was at a “hot spot” four years later that a SWOP counsellor reached out. Through the program, she got sober, met the teenage boy orphaned and ostracized by AIDS who would become her adopted son, and found her voice. “SWOP has empowered me to know my potential. What I’m able to do and what I’m not able to do—I’m not able to violate anybody’s rights.”
She loses clients when she tells them she’s HIV-positive. Sometimes they call her a killer. “Many walk away. Some appreciate it and give a token $1 or $2. Others can abuse you. Or others say you are denying them,” Adhiambo says.
But she spreads the word among her fellow sex workers: “Disclosure is the key to prevention.” On antiretroviral therapy for 14 years, and with a viral load currently undetectable, Adhiambo feels healthy.
“I’m always laughing. I am a very jovial mother, a very happy mother, a very positive mother.”
And life goes on.



















Thanks to U M for publishing my story that has also inspired me.Let us all walk the path together to prevention intervention on hiv,tb and the law.I wish to visit the university of Manitoba one day to meet you guys physically.cheers.!
Amazing.
Thanks you, for all the work you put in HIV/AIDs.In Western Kenya many have been affected/infected.Keep up the good work
These are such inspiring stories. I admire you, Joyce – and others who are so devoted and do not quit – on the contrary. You have no idea how much you are inspiring human beings.
Thanks Celline,for I am committed to positive health and dignity prevention in my community .
What an amazing story about the crucial partnership between U of M and U of N. Thank you to all that shared their contribution to the fight against HIV/AIDS.
Big up guys you’re awesome and hard working,you have brought change in our lives as sex workers in prevention of HIV and us who are living positively.
Great work and the story is making the world a better place.Congrats for the courage to share.
Thanks Joyce and Rosemary for sharing your story. Very inspiring. Continue with the great work.
You are a true hero!Bravo!
Wow! nice article and keep it up